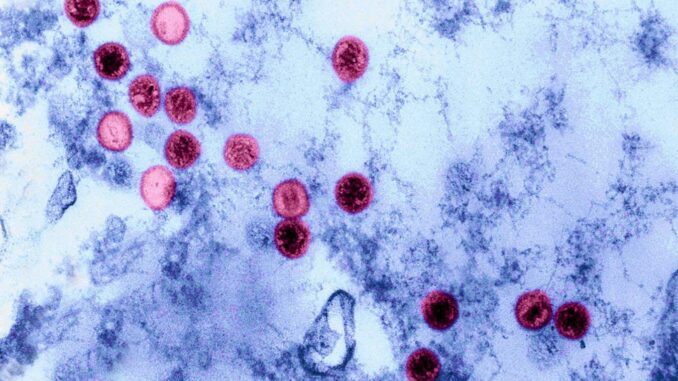
Epstein-Barr virus is a very common infection, but that doesn’t mean it’s harmless
Science History Images/Alamy
About 1 in 10 people carry genetic variants that make them particularly vulnerable to the Epstein-Barr virus (EBV), a ubiquitous pathogen increasingly linked to conditions such as multiple sclerosis and lupus. The finding, which comes from a study of more than 700,000 people, may help explain why EBV causes serious illness in some people while leaving most of us virtually unharmed.
“Almost everyone is exposed to EBV,” he says Chris Wincup at King’s College London, who was not involved in the research. “How is it that everyone is exposed to the same virus and it causes an autoimmune condition, and yet most people don’t end up with an autoimmune disease?” This study offers an answer, he says.
The Epstein-Barr virus was first described in 1964 after scientists found its particles in a type of cancer called Burkitt’s lymphoma. We now know that more than 90 percent of people are infected with EBV at some point because almost everyone makes antibodies against the virus.
In the short term, EBV is the main cause of infectious mononucleosis, also known as mono or glandular fever, which usually goes away after a few weeks. In some cases, EBV appears to contribute to serious long-term autoimmune conditions in which the immune system attacks the rest of the body. For example, a 2022 study provided strong evidence that it is a major cause of multiple sclerosis, in which the protective coverings around nerves are damaged, leading to difficulty walking.
“Why is it possible that people at the population level respond so differently to the same viral infection?” he says Caleb Lareau at Memorial Sloan Kettering Cancer Center in New York.
To find out, Lareau and his colleagues examined health data from more than 735,000 people from the UK Biobank study and an American cohort called All of Us. Participants had their genomes sequenced – crucially, this was done using blood samples. “When EBV infects, it actually leaves a copy of itself in some cells” in the blood, Lareau says. This means that the human genomes in the study samples contained copies of the EBV genome.
The researchers found that some people had much more EBV DNA than others: 47,452 study participants (9.7 percent) had more than 1.2 complete EBV genomes for every 10,000 cells. This means that while most participants largely cleared the virus after infection, this group did not.
Next, the team tried to find out why these people are more vulnerable to EBV. “Were there certain differences in their genome that predisposed them to higher levels of EBV?” says a team member Ryan Dhindsa at Baylor College of Medicine in Houston, Texas. “We found that there were 22 different regions of the genome that were associated with higher levels of EBV,” he says. “Encouragingly, many of those genomic regions that emerged have previously been associated with various immune-mediated diseases.”
The strongest associations were with genes that code for the major histocompatibility complex, a set of immune proteins that play a large role in distinguishing between the body and invading pathogens. “There were certain people who had different variants in their major histocompatibility complex,” says Dhindsa. Further experiments suggested that these variants affected the body’s ability to detect EBV infection.
“This virus does something to our immune system, and in some people it does something permanent and permanent to our immune system,” he says Ruth Dobson at Queen Mary University of London. When viral DNA persists, it can gently nudge the immune system and eventually trigger it to attack the body, he says.
Finally, the genetic variants that have been linked to high levels of EBV have also been linked to many other traits and conditions – notably a higher risk of autoimmune conditions such as rheumatoid arthritis and lupus, adding to the evidence that the virus is involved.
The team also found an association between these variants and illness or fatigue. This was interesting because some studies suggest that EBV could be a causative factor in myalgic encephalomyelitis, also known as chronic fatigue syndrome (ME/CFS). Because of the huge sample size, “we can say with confidence that the signal is there,” says Dhindsa. “But we don’t know exactly what the relationship is at this point.
For Wincup, a key benefit of the results is pinpointing which parts of the immune system are disrupted by persistent EBV. Specific treatments could then target these components, potentially reducing the damage caused by EBV-related conditions.
Another option is to vaccinate people against EBV. Only experimental vaccines have been developed so far. Vaccination against EBV would be a radical step, says Wincup. “Many people see EBV as a fairly benign disease,” he says. However, the conditions associated with it take a huge toll on a significant number of people. “So how is it benign?”
topics:

Leave a Reply