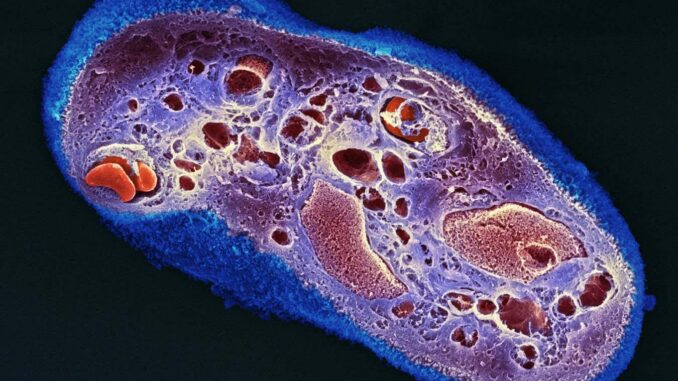
Scanning electron micrograph of a section of a human placenta
Scientific Photo Library
According to research in mice and humans, skin wounds heal with less scarring when thin slices of dried human placenta are applied as dressings.
The healing properties of placenta have been known since at least the early 20th century, when the tissue was sometimes applied to burns to reduce scarring. However, the treatment fell out of favor due to the potential risk of disease transmission.
Now, with new methods of safely sterilizing and preserving placentas, such dressings are gaining attention again. In particular, the researchers investigated the healing properties of the amniotic membrane, the innermost layer of the placenta, which forms the fetus during pregnancy and contains a rich variety of growth factors and immunomodulating proteins.
Several US companies have begun collecting amniotic membranes from placentas donated after elective cesarean sections. They peel this thin membrane from the rest of the placenta, freeze dry it, cut it into standard sizes, wrap it, and sterilize it with radiation. This preserves its growth factors and other medicinal substances and at the same time destroys any pathogens. The resulting tissue paper-like sheets can then be used as wound dressings.
To see if they reduce scarring, Geoffrey Gurtner at the University of Arizona and his colleagues made surgical incisions on the backs of anesthetized mice and used a device to pull on the sides of the wounds and slow the healing process.
When left untreated, the wounds healed poorly, with large, lumpy scars. In contrast, when dressings made from human amniotic membrane were applied, the wounds healed much better, with thinner, flatter, barely visible scars. The dressings did not cause adverse reactions in the mice because the placenta had “immune privilege,” a condition that prevents the immune system from attacking.
Some American surgeons and doctors are already experimenting with using amniotic membrane dressings on people’s wounds as the Food and Drug Administration authorizes their clinical use. For example, they are applied to surgical wounds and chronic, non-healing wounds caused by conditions such as diabetes.
ON studies which came out in June 2025 gave us an idea of how well these dressings work in a real clinical setting. Ryan Cauley at Beth Israel Deaconess Medical Center in Boston, and colleagues combed through a large US database of anonymous patient medical records to identify 593 people who received amniotic membrane dressings to treat chronic wounds or burns and compared them with 593 similar individuals who received other treatments.
The researchers found that wounds treated with amniotic membrane dressings were less prone to infection and the development of thick, raised scars, known as hypertrophic scars. This confirms the growing popularity of these dressings, although Cauley and his colleagues note in their paper that “further prospective, randomized studies with extended follow-up are warranted to confirm these findings.”
Meanwhile, other groups are investigating the potential of placental tissue to treat organs other than the skin. For example in 2023 Hina Chaudhry at the Icahn School of Medicine at Mount Sinai in New York and her colleagues found that injections of placental cells repaired heart injuries in mice, suggesting they may one day be used to treat damage caused by heart attacks.
topics:

Leave a Reply