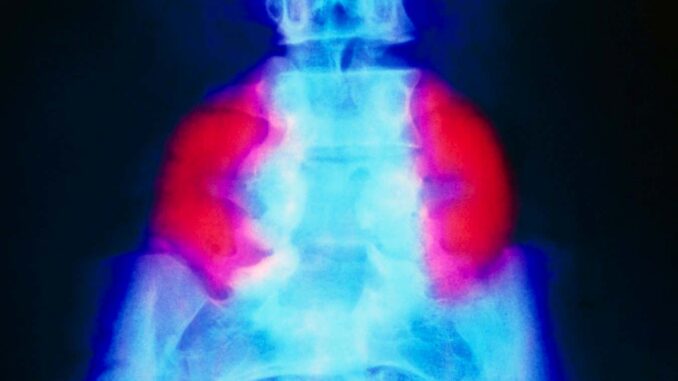
False color x-ray showing a large neural tube defect (red) on both sides of the lower back in someone with spina bifida
LIBRARY OF SCIENTIFIC PHOTOGRAPHS
A patch made from stem cells from a donor placenta has been used to treat fetuses in utero with severe spina bifida in a world-first study. The new approach appears to have reversed the brain complication linked to the congenital condition at least as effectively as conventional treatment, but is expected to enable more children to walk in the long term.
The mother of one, now 4, says she expected her son Toby to need a wheelchair when he was diagnosed with the condition in utero. “But Toby is healthy. [and] he’s hit all his milestones – he’s walking, running and jumping – and has no issues with bladder control, which is rare for people with this condition,” she says.
Spina bifida – which affects approx 1 in every 2,800 births in the US each year – occurs when the baby’s spine and spinal cord do not fully develop in the womb. In the most severe form of the disease, called myelomeningocele, the spinal cord and surrounding tissue protrude from the gap in the vertebrae, often impairing bowel and bladder motility and control. The cause of spina bifida is unknown, but folic acid deficiency during pregnancy increases the risk.
One of the standard treatments involves surgery in utero to tuck the spinal cord and surrounding tissue back into the vertebrae, before stitching the skin together to create a tight seal. “But a lot of kids still can’t walk and that’s the way it is.” [usually] no improvement in bowel or bladder control,” he says Diana Farmer at the University of California, Davis.
This led Farmer and his colleagues to consider whether adding stem cells might help by promoting the growth and repair of spinal cord tissue. To find out, they recruited six pregnant women carrying fetuses with myelomeningocele.
At about 24 weeks gestation, all fetuses develop a common complication called hindbrain herniation, where too much fluid builds up in the skull, pushing the lower part of the brain, the cerebellum, through a hole in the base of the skull. Standard surgery often helps reverse hindbrain herniation, but many children still have complications.
In the latest study, all the fetuses underwent standard surgery, but also received a patch several centimeters long containing stem cells obtained from donated placentas, which were embedded in a matrix of sticky proteins. Surgeons placed this patch on the spine before the skin was sewn around it. “Cells secrete magic stem cell juice,” Farmer says.
At birth, the surgical site healed well in all children, with no evidence of abnormal cell growth. “The key concern was that adding stem cells to a fetus would cause the cells to grow like crazy, but we haven’t seen that,” Farmer says. MRI scans of their brains also showed that the treatment completely reversed the hindbrain herniation.
“My personal opinion is that it will improve long-term outcomes compared to the standard approach [based on evidence from animal studies],” he says Panicos Shangaris at King’s College London.
The researchers hope to evaluate this in a study where 35 fetuses with myelomeningocele will receive a stem cell patch and compare their results to a previous study that used conventional surgery, Farmer says.
But Shangaris says a better comparison, more likely to lead to treatment approval, would be to compare the two approaches in a head-to-head trial that evaluates their safety and effectiveness in fetuses randomly assigned to each intervention.
topics:

Leave a Reply